Health
10 things to know about the deadly Monkey Pox
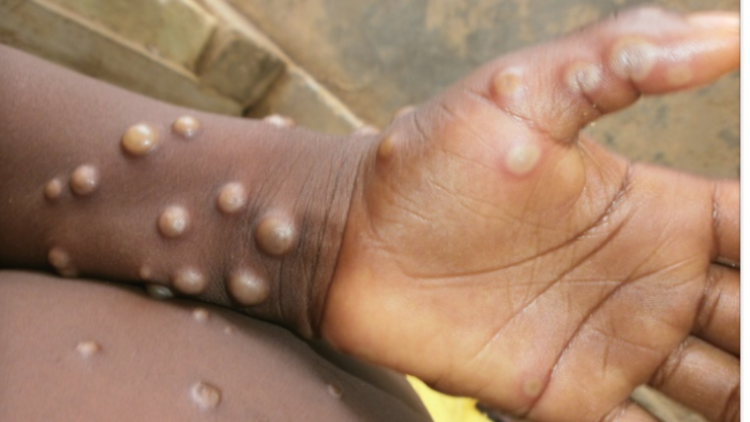
There seems to be a widespread panic over the deadly Monkey pox virus and rightly so. At the moment, no specific treatment is recommended for monkey pox, NewsWireNGR will be telling you all you need to know as part of our information and advocacy outreach and in telling under-reported stories to not only inform our readers but educate members of the public.
The Nigeria Centre for Disease Control has registered 59 suspected cases of Monkeypox with 15 confirmed, its Director-General, Dr Chikwe Ihekweazu, said on Tuesday in Abuja, Nigeria.
Ihekweazu was reacting to the Dallas, Texas resident who recently returned from Nigeria and tested positive to the disease.
The News Agency of Nigeria reports that it was the first confirmed case of the virus in the U.S. since 2003 – Laboratory tests confirmed that the patient was infected with a strain of the virus mainly seen in West Africa, which included Nigeria.
With passengers wearing masks on the flight and in the airport, the health department said that the risk of spreading monkeypox via respiratory droplets to others on the planes and in the airports was low.
But according to the World Health Organization, Monkeypox virus is mostly transmitted to people from wild animals such as rodents and primates, but human-to-human transmission also occurs.
WHO explains that Monkeypox virus is transmitted from one person to another by contact with lesions, body fluids, respiratory droplets and contaminated materials such as bedding.
Monkeypox is a viral zoonosis (a virus transmitted to humans from animals) with symptoms similar to those seen in the past in smallpox patients, although it is clinically less severe. With the eradication of smallpox in 1980 and subsequent cessation of smallpox vaccination, it has emerged as the most important orthopoxvirus. Monkeypox occurs in Central and West Africa, often in proximity to tropical rain-forests.
Treatment and vaccine
There is currently no specific treatment recommended for monkeypox. Vaccination against smallpox with vaccinia vaccine was demonstrated through several observational studies to be about 85% effective in preventing monkeypox. Thus, prior childhood smallpox vaccination may result in a milder disease course.
However at the present time, the original (first-generation) smallpox vaccines are no longer available to the general public. A newer vaccinia-based vaccine was approved for the prevention of smallpox and monkeypox in 2019 and is also not yet widely available in the public sector.
Prevention
Raising awareness of risk factors and educating people about the measures they can take to reduce exposure to the virus is the main prevention strategy for monkeypox. Scientific studies are now underway to assess the feasibility and appropriateness of using vaccinia vaccine for the prevention and control of monkeypox. Some countries have, or are developing, policies for use of vaccinia vaccine to prevent infection, for example in laboratory staff and health workers who may be at risk of exposure.
Key facts
Monkeypox is caused by monkeypox virus, a member of the Orthopoxvirus genus in the family Poxviridae.
Monkeypox is a viral zoonotic disease that occurs primarily in tropical rainforest areas of Central and West Africa and is occasionally exported to other regions.
Monkeypox typically presents clinically with fever, rash and swollen lymph nodes.
Monkeypox virus is mostly transmitted to people from wild animals such as rodents and primates, but human-to-human transmission also occurs.
Monkeypox virus is transmitted from one person to another by contact with lesions, body fluids, respiratory droplets and contaminated materials such as bedding.
Typically, up to a tenth of persons ill with monkeypox may die, with most deaths occurring in younger age groups.
The clinical presentation of monkeypox resembles that of smallpox, a related orthopoxvirus infection which was declared eradicated worldwide in 1980.
Vaccinia vaccine used during the smallpox eradication programme was also protective against monkeypox. A new third generation vaccinia vaccine has now been approved for prevention of smallpox and monkeypox. Antiviral agents are also being developed.
Signs and symptoms
The incubation period (interval from infection to onset of symptoms) of monkeypox is usually from 6 to 13 days but can range from 5 to 21 days.
The infection can be divided into two periods:
- the invasion period (lasts between 0-5 days) characterized by fever, intense headache, lymphadenopathy (swelling of the lymph nodes), back pain, myalgia (muscle aches) and an intense asthenia (lack of energy). Lymphadenopathy is a distinctive feature of monkeypox compared to other diseases that may initially appear similar (chickenpox, measles, smallpox).
- the skin eruption usually begins within 1-3 days of appearance of fever. The rash tends to be more concentrated on the face and extremities rather than on the trunk. It affects the face (in 95% of cases), and palms of the hands and soles of the feet (in 75% of cases). Also affected are oral mucous membranes (in 70% of cases), genitalia (30%), and conjunctivae (20%), as well as the cornea. The rash evolves sequentially from macules (lesions with a flat base) to papules (slightly raised firm lesions), vesicles (lesions filled with clear fluid), pustules (lesions filled with yellowish fluid), and crusts which dry up and fall off. The number of the lesions varies from a few to several thousand. In severe cases, lesions can coalesce until large sections of skin slough off.
Monkeypox is usually a self-limited disease with the symptoms lasting from 2 to 4 weeks. Severe cases occur more commonly among children and are related to the extent of virus exposure, patient health status and nature of complications. Complications of monkeypox can include secondary infections, bronchopneumonia, sepsis, encephalitis, and infection of the cornea with ensuing loss of vision.
People living in or near forested areas may have indirect or low-level exposure to infected animals, possibly leading to subclinical (asymptomatic) infection.
The case fatality ratio of monkeypox has varied between 0 and 11 % in the general population, and has been higher among young children. In addition, persons younger than 40 or 50 years of age (depending on the country) may be more susceptible to monkeypox as a result of the termination of routine smallpox vaccination worldwide after the eradication of smallpox.






