Breaking News
“No Doctors When I Was Having My Daughter” – The Dying Mothers of Okearo, Ogun State
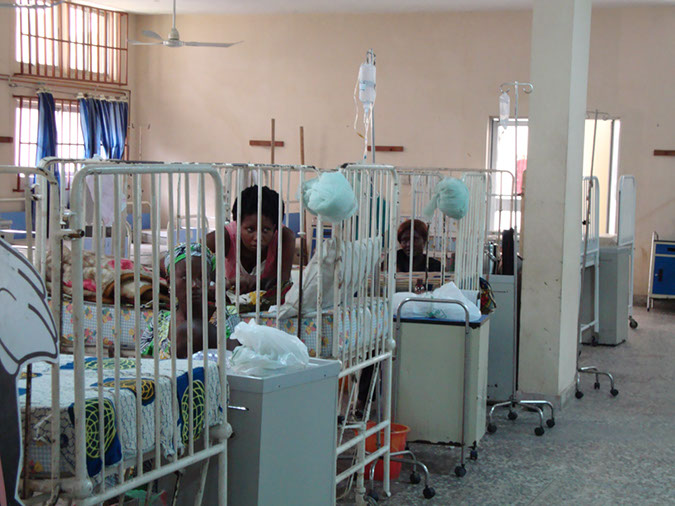
by Oluwatosin Adeshokan
In a dimly lit shop in Okearo as Adeleye Dopemu tended to Fiyin her fifteen month old daughter for a new bump on her head from falling, her newest daughter Esther laid on the floor crying. Esther was five months old, but weighed four and a half kilograms. The recommended weight for children her age is between 5.1 – 8.1kg.
Adeleye said her daughter has not had her immunizations since she was born. As at the time Adeleye went into labour with Esther, she had not registered at any hospital for pregnancy care. Instead, she had been having irregular meetings with an “Aunty nurse” that lived two streets away from her house in Okearo.
Aunty nurse, had not provided her with standard antenatal care, meaning Adeleye received no essential medicines or advice on how to deal with her pregnancy. Her ten month daughter Fiyin was handed over to her neighbour and she made her way to the nurse’s house for delivery. She delivered her Esther; a 2 kg baby just as soon as she got to the delivery room, but immediately passed out.
Months before she delivered her baby, she had fallen out with her husband and could barely fend for her other two children. After she was revived, Aunty Nurse contacted her sisters to come take her away. The delivery took a toll on her health and threatened her life. “She was a very skinny when we were called to pick her up. Her baby was extremely tiny and underweight. She was skinnier than we left her and was almost dead when we went to get her.” Her sister Adebimpe Adewole told me.
The cost of good maternity health care
On the average there are 8.14 maternal deaths per one thousand live births in Nigeria, compared to Sub Saharan Africa’s rate at 5.2. going by the CIA factbook data.
According to Dr. Olaokun Soyinka the former commissioner for Health in Ogun state in 2015 claimed that maternal mortality rates in the state had reduced from 2.95 to 2.45 deaths per live births. But a 2012 study on maternal mortality rates using Olabisi Onabanjo University teaching Hospital medical record of 10 years 2001 to 2010 by Olukoya Oludare Agnes and A. A. Sodipo, the maternal mortality rate in 2010 was 7.48 deaths per thousand deaths in the hospital.
Adeleye lives in Okearo, a community with proximity to Lagos and would neither qualify to be described as either urban or rural. “We have been told that Okearo will develop, but since I was a child, it has not developed. We have roads, but they are bad. We have electricity, but we don’t quite have electricity. We are so close to Lagos and its development, but we are not as developed.” Oghenekaro Otitifore, a teacher in Okearo said. For the purposes of planning healthcare delivery, the Ogun State government grouped Okearo and Ibaragun together as a zone. Though 52 medical centres including hospitals, clinics, maternity and diagnostic centres serve the populace, there are no secondary public health centers. The closest glimpses of hope for expectant mothers unable to afford the private health centers in Okearo are in Lagos; the General hospital at Ifako and the Lagos State University Teaching hospital in Ikeja. Okearo is 4 km’s away from the General hospital in Ifako, Lagos, but what will be a twenty minute drive usually turns to a two hour bus ride.
Unable to afford the cost of maternity care, women in communities like Okearo are left with fewer and sometimes unsafe options. Despite the presence of two primary health centers to serve all of Okearo including Matogun, Lambe and Farm in Gudugba and Yewande, general trust of the health centers especially among pregnant women and nursing mothers is very low. Okearo is one of the biggest towns in Ifo Local government that has an estimated population of 750,000 in 2016. When Bukola Benson; a stay at home mother of four daughters was pregnant with her last daughter; Serena, she quickly checked herself into a Private hospital. She paid five hundred naira every two weeks from the third month of her pregnancy as part of the antenatal costs. She also had to pay one thousand five hundred naira for the tetanus toxoid injection.
“There are no doctors in the clinics in Gudugba and Yewande. When I was having my first daughter, we did not live in Okearo, we lived in Gbagada and it was a private hospital. I bled and bled so much that I needed a doctor immediately. I nearly died. Now, I know that I will bleed after my delivery, so I just register at a private hospital where I am sure I can see a doctor.” Bukola said.
Mrs. Esther Olowokere, a midwife that runs her own Mission Birth outfit shared this sentiment. “Most people can’t afford the general hospitals and the attitude of the nurses in the health centers are just terrible.” Mrs. Esther said.
A Better Alternative?
In 2013, a program by the Oyo State Ministry of Health trained women in Midwifery and gave them certificates. The training took place for six months after which they went on internships with hospitals for twelve to eighteen months. “Most people don’t want to deliver in a place where there’s no electricity and where the nurses will shout at them. They want prayers and peace of mind. While the hospitals charge as much as thirty thousand naira, we charge five thousand naira for deliveries and if the deliveries have complications, we charge ten thousand naira. We take care of all of our patients needs and use our generator for the delivery.” But sometimes there are complications. Mission Birth Attendants usually have arrangements with private hospitals and doctors to deal with these problems. In a lot of ways, Mission Birth attendants that dot Okearo and its environs are better qualified to handle childbirth as well as complications that arise from childbirth better than the government provided health centers.
Ideally, the primary health centers should be equipped to deal with births and arising complications. But there is a bias against these primary health centers. According to Dr. Femi Pope, “In an ideal world, primary health centers have proper equipments like Partographs to track the vitals of mother and child to reduce cases of infant and maternal mortality, but these partographs are in most secondary health centers and teaching hospitals defeating the purpose for which it was made.” While Dr. Femi Pope believes a lot of fear against public hospitals and doctors, some of these fears are unfounded. According to him, “Nigeria does not have a competence problem, Nigeria has a facility and manpower problem. Nigerian doctors are not getting paid well enough, some aren’t getting paid at all. Nigeria is exporting more doctors these days than she’s producing.” An improper referral system makes primary health centers . The lack of medical planning by state governments in Nigeria as well as a failure to implement Universal healthcare in Nigeria broadens the divide between poor citizens that can’t afford private hospitals and the public primary healthcare.
Earlier this year, two women died on the way to hospitals from the traditional birth attendants home office. The deliveries were successful until the women could not stop bleeding. The bad road from Matogun to Okearo meant they could not get to the hospital in time. The roads still remain terrible, the public health centers retain their rundown aesthetic, inside there are few doctors to deal with so many patients. Ibikunle Amosun, the governor of Ogun State presented a budget proposal of N221.129 billion to the state House of Assembly for approval. Of this, only 6.8% of this amount was budgeted for healthcare. An official at the Ogun State Ministry of Health, said to me, “This budget does not really care to solve problems that are developing. This government has its priorities at other places and projects, so this budget pays the salaries and does little renovation. “
For women like Adeleye and Bukola, health care by the government is non existent. The government can not be depended on for the provision of health care and a lot of other social amenities that are commonplace in other parts of the world.






